The Disease that 150,000 Australians are unaware they may have
Identifying the early symptoms and those who are most at risk from Glaucoma
by Dr. Aparna Raniga MBChB FRANZCO

It is estimated that there are 300,000 Australians living with glaucoma but up to 50% are undiagnosed. In developing countries meanwhile, it is estimated that as many as 90% of glaucoma cases are undiagnosed.
The statistic is a frightening one since glaucoma is the leading cause of irreversible blindness worldwide. It is estimated that 5.9 and 5.3 million people will suffer from blindness secondary to primary open- and closed-angle glaucoma, respectively, in 2020. [i]
Glaucoma is not one specific condition but rather a group of diseases characterised by progressive optic neuropathy due to loss of neural tissue and a posterior bowing of the lamina cribrosa. It is defined as a progressive optic neuropathy which are characterised by specific structural changes in the optic disc and specific functional defects detected by automated visual field testing. Elevated intraocular pressure is an important risk factor but is not a defining characteristic of the disease. [ii]
Primary open-angleglaucoma (POAG) v Primary angle-closure glaucoma (PACG)
There are several types of glaucoma with Primary Open-angleGlaucoma (POAG) being the most common. In POAG, there are characteristic optic nerve changes (damage) associated with open angles (the area between the iris and cornea) and elevated eye pressure. POAG can occur at any age, but the incidence and prevalence increases with age. Even with treatment, 15% of patients become blind in at least one eye in 15 to 20 years of follow-up. [iii]
Although Primary Open-angle Glaucoma (POAG) is the more common, Primary Angle-closure Glaucoma (PACG) is more severe and more likely to result in blindness if not treated properly. PACG represents approximately 25% of all cases of glaucoma worldwide but is responsible for about 50% of blindness induced by glaucoma. In China, primary angle closure glaucomahas caused unilateral blindness in 1.5 million individuals and bilateral blindness in a further 1.5 million individuals. [iv]
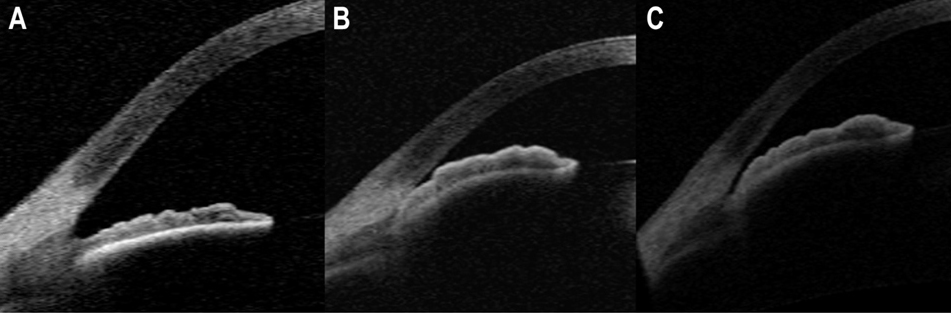
Anterior segment OCT illustrating an open angle in image A and a closed angle in images B and C. Courtesy of SassanMoghimi, MD in Contemporary approach to the diagnosis and management of primary angle-closure disease M. Reza RazeghinejadMD Jonathan S.Myers MD Survey of Ophthalmology Volume 63, Issue 6, November–December 2018, Pages 754-768
Risk profiling in Glaucoma
Everyone is at risk ofglaucoma but some are more at risk than others. Ocular risk factors include the following:
- Intraocular pressure (IOP) – POAG can develop at any IOP. Indeed, there is strong evidence that a higher mean IOP at diagnosis or follow up is a risk factor for development and progression of glaucomatous damage.
- Central corneal thickness (CCT) – A thin CCT is an important predictive factor for Glaucoma development and in ocular hypertensives and Glaucoma suspects
- Myopia – Individuals with myopia have a greater risk of developing open angle Glaucoma, with the risk being greater in high myopia
- Disc haemorrhage – The presence of a disc haemorrhage is associated with an increased risk of developing Glaucoma and is a marker for Glaucoma progression
Systemic risk factors meanwhile include the following:
- Increasing age – incidence and prevalence of both open and closed angle Glaucoma increases with age
- Ethnicity – POAG has an increased incidence and prevalence in those of African ancestry, Hispanics and Caucasians. Angle closure Glaucomameanwhile has an increased incidence and prevalence in those of Asian descent
- Family history – first degree relatives have an up to 25% chance of developing Glaucoma and screening is recommended
- Blood pressure (BP) – Lower nocturnal BP is associated with higher POAG incidence and prevalence across all racial groups
- Diabetes mellitus – increases the risk of Glaucoma onset
Symptoms and the impact on a patient’s quality of life
Most field defects are negative scotomas which are not perceived. That said, they may be perceived as darker or blurred areas. This is because the brain will cause so called “filling-in” which creates an inaccurate but “believable” image in the part of the patient’s visual field that is defective. This is best explained by the images below.
In a study by Crabbe et al, patients with moderate to advanced glaucoma were presented the images below and asked to select the image that best reflected their vision. 25% of patients chose the image on the top left, indicating no perceptual changes. 54% of patients chose the image depicting blurred parts (bottom left), and 15% selected the image depicting missing parts (bottom right). None selected the images depicting black parts.[v]

The impact on one’s quality of life can be immense. Glaucoma progression is associated with decreased reading speeds. Improving contrast with better lighting however sometimes helps to improve reading
Social interactions are also often impacted. Patients with advanced glaucoma may be limited by poor facial recognition. Self-confidence can in turn be affected whilst progressive glaucomatous visual field loss is often associated with frailty, cognitive decline, Alzheimers disease and higher mortality.
Mobility is also impacted as the visual field loss restricts physical activity. The disease is associated with a higher rate of falls, especially a higher rate of falls per step taken. There is certainly a greater risk of falls at home, even though fewer steps are taken at home.Glaucoma patients may benefit from modifying their home environment and improve lighting to prevent such falls.Driving is also impacted and there is an increased likelihood of being unable to drive with progressive glaucomatous visual field loss.
Whilst there is no cure for glaucoma, the disease can be controlled however and further loss of sight either prevented or slowed down considerably. Essentially it is a condition that can be managed effectively with the right treatment and/or surgery but being aware of the symptoms and identifying and treating those at risk as early as possible is the absolutely key.
SOURCES:
- D.S. Friedman, P.J. Foster, T. Aung, M. He Angle closure and angle-closure glaucoma: what we are doing now and what we will be doing in the future ClinExpOphthalmol, 40 (4) (2012), pp. 381-387.
- P.J. Foster, R. Buhrmann, H.A. Quigley, G.J. Johnson The definition and classification of glaucoma in prevalence surveys Br J Ophthalmol, 86 (2002), pp. 238-242.
- Rate of visual field loss and long-term visual outcome in primary open-angle glaucoma. Kwon YH, Kim CS,Zimmerman MB, Alward WL, Hayreh SS Am J Ophthalmol. 2001 Jul; 132(1):47-56. Glaucoma clinical trials and what they mean for our patients. Lichter PR Am J Ophthalmol. 2003 Jul; 136(1):136-45.
- P.J. Foster The epidemiology of primary angle closure and associated glaucomatous optic neuropathy SeminOphthalmol, 17 (2) (2002), pp. 50-58.
- Source: Crabbe et al, Ophthalmology 2013, Patient perception of visual field loss.

Dr. Aparna Raniga
MBChB FRANZCO





