Arthroscopic Rotator Cuff Repair

Rotator Cuff Tear
by Dr Kalman Piper
Sydney Orthopaedic Shoulder Surgeon
Dr Kalman Piper is a highly experienced, Sydney based, orthopaedic surgeon who can offer a complete range of treatment options for all upper limb conditions. He has a subspecialty interest in shoulder surgery and has advanced training in arthroscopic surgery.
Here, he takes us through The Rotator Cuff, how it is diagnosed, treated and repaired.
What Is The Rotator Cuff?
The shoulder is a ball and socket joint; however the ball (humeral head) is relatively large, compared to the socket (glenoid). This gives the shoulder a large range of motion compared to other, more constrained ball and socket joints in the body, such as the hip joint.
Attached to the humeral head is a group of four tendons that rotate the humeral head on the glenoid and therefore, move the arm. The four tendons are collectively called the rotator cuff. The functions of the tendons of the rotator cuff vary depending on where they attach to the humeral head. The supraspinatus tendon attaches to the top of the humeral head. When it pulls on the humeral head it elevates the arm. It is the most common tendon involved in rotator cuff tears. The subscapularis tendon attaches to the front of the humeral head and internally rotates the shoulder. There are two tendons, infraspinatus and teres minor, attached to the back of the humeral head which externally rotate the shoulder.
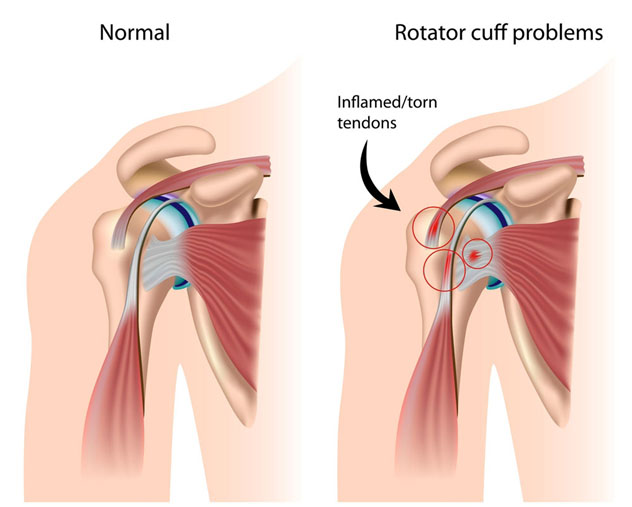
What Is A Rotator Cuff Tear?
A rotator cuff tear is detachment of one or more of the tendons of the rotator cuff, from the insertion into the bone of the humeral head. A tear can be a result of an injury to the shoulder (e.g. while lifting or during a fall), but many tears develop slowly and often patients cannot recall any specific injury to the shoulder. Rotator cuff tears are very common and usually occur in patients over the age of 40 years. The symptoms of rotator cuff tear vary from patient to patient, but usually involve weakness of the shoulder and pain. The pain is often felt during attempted elevation of the shoulder, lifting, driving or with overhead activities. Pain is often present at night and may disturb sleep.
The tear may involve a part of the tendon (partial tear), all of the tendon (full thickness tear) or more than one tendon (massive rotator cuff tear). When the tendon is completely torn, the tendon end retracts away from the bone insertion due to the pull of the muscle attached to the other end. A massive, retracted tear may not be repairable if it has been present for a long time.
How Is A Rotator Cuff Tear Diagnosed?
A clinical examination may indicate a rotator cuff tear, however the diagnosis is usually confirmed with x-rays and a MRI scan. A MRI will also help determine the size of the tear and the amount of retraction of the tendon end.
An ultrasound scan can also be used to diagnose a rotator cuff tear, however they are not as accurate as an MRI scan, nor can they be used to plan surgery. MRI will also be able to detect other common conditions associated with rotator cuff tear.
Other Common Conditions Associated With Rotator Cuff Tears:
Rotator cuff tears are commonly associated with:
- Damage to the long head of biceps.
- Shoulder impingement.
- AC Joint arthritis
The long head of biceps enters the shoulder joint adjacent to the supraspinatus tendon and is often damaged with the rotator cuff. Also, once the rotator cuff is torn, the torn tendon end can rub on the undersurface of the acromion (bone above the shoulder). This is called sub acromial impingement and can be very painful.
Arthritis of the AC Joint can also be seen on an MRI scan, and is common in patients with a rotator cuff tear, although it is usually not related to the development of rotator cuff tear.
All these conditions can be treated at the same time as the rotator cuff tear.
How Is A Rotator Cuff Treated?
There are several treatment options available for rotator cuff tears. These include:
- A period of rest in a sling, followed by physiotherapy.
- Injections into the shoulder to treat pain and inflammation.
- Arthroscopic surgery for rotator cuff repair
- Joint replacement surgery (reverse shoulder replacement) for massive, irreparable cuff tears. The best treatment choice will be determined by several factors including the size of the tear, the retraction of the tear, how long the tear has been present (chonicity), your age, and the functional demand on the shoulder.
Arthroscopic Rotator Cuff Repair
The rotator cuff has a broad insertion into a prominence of bone of the humeral head called the tuberosity. Rotator cuff tears usually occur at this site, with the tendon end detaching from its bony insertion or “footprint”. Rotator cuff surgery may be necessary if your shoulder is painful or weak. The surgery can usually be performed using keyhole or arthroscopic techniques.
To perform an arthroscopic rotator cuff repair small incisions or portals are made around the shoulder and a thin, pencil like camera is inserted. Saline is pumped into the shoulder joint to maintain a clear view of the shoulder. Instruments are inserted via portals and the surgery is performed whist observing the camera image on a monitor.
The first step of the repair is to prepare the footprint for tendon reattachment. Scar tissue is removed from the footprint to allow the tendon to directly oppose the bone. Following preparation of the footprint, the tendon is reattached to the bone using a variable number of suture anchors.
A suture anchor is a small screw approximately 5mm in diameter. It is screwed into the bone until the whole screw lies within the bone and there is no prominence. The screw has an eyelet, through which passed strong suture material. The suture is then passed through the torn tendon, and a knot is tied to oppose the tendon to the footprint. For larger tears, a series of anchors and sutures are linked to increase the area of tendon opposed to the footprint.
In addition, an acromioplasty is usually performed. An acromioplasty involves removal of a spur of bone from the under surface of the acromion, the bone over the shoulder joint. The bone spur is removed to prevent impingement or catching of the rotator cuff during shoulder elevation. The acromioplasty is performed with a small bur, approximately 4mm in diameter. Usually, only a few millimetres of bone is removed.
The suture repair construct maintains contact between the tendon and the bone while the tendon heals. Because the tendon has been previously torn, the tendon ends are friable and it is possible the sutures can cut out of the tendon. Therefore, the shoulder is immobilised in a sling for a period of six weeks, to protect the repair. During this time, limited range of motion exercises are performed to prevent the onset of frozen shoulder. It is critical in the first six weeks that all exercises are “passive”, which means the repaired tendon is not used to move the arm while it is healing.
Following six weeks of immobilisation, the tendon has healed sufficiently to allow active range of motion exercises, coordinated by a physiotherapist. Strengthening exercises are delayed for three months, to allow the rotator cuff repair to consolidate.
Dr Kalman Piper
MBBS FRACS (Orth)
Dr Piper was born in Brisbane, and graduated in Medicine & Surgery from the University of Queensland. He completed Orthopaedic training in Sydney, with the Australian Orthopaedic Association and was awarded Fellowship of the Royal Australian College of Surgeons (FRACS) in 2009.
Dr Piper was then accepted to undertake training in advance shoulder surgery in France with Dr Laurent Lafosse, a world leader in arthroscopic shoulder surgery. The experience he gained in France is unmatched anywhere in the world, and has allowed Dr Piper to offer new and innovative techniques in Australia.
Dr Piper is passionate about teaching and training surgeons, and passing on the knowledge he has obtained. He has been appointed an honorary position as a clinical lecturer at Macquarie University, and is extensively involved with the teaching and training of international orthopaedic surgeons enrolled in the Masters of Advanced Surgery at the University. He also trains Australian doctors on the Australian Orthopaedic Training Program.
To book a consultation and to contact Dr Piper:-
T: 1800 746 853
reception@kaliper.com.au
www.kaliper.com.au
Lakeview Private Hospital
Suite 1, Level 1
17 – 19 Solent Circuit
Norwest NSW 2153
Macquarie University Clinic
Suite 303, Level 3
2 Technology Place
Macquarie University NSW 2109





