Colorectal lesions and cancer screening
Dr Farzan Bahin
MBBS (Hons), FRACP, PhD, MPhil (Med)
Despite being a mostly preventable malignancy, Australia has one of the highest rates of colorectal cancer (CRC) worldwide. One in 13 Australians develop CRC in their lifetime, making it the second most common cause of cancer related death in Australia. These somewhat opposing aspects relate to inadequate uptake of CRC screening, misconceptions about screening options and technical aspects such as missed or incompletely resected pre-cancerous lesions leading to interval cancer.
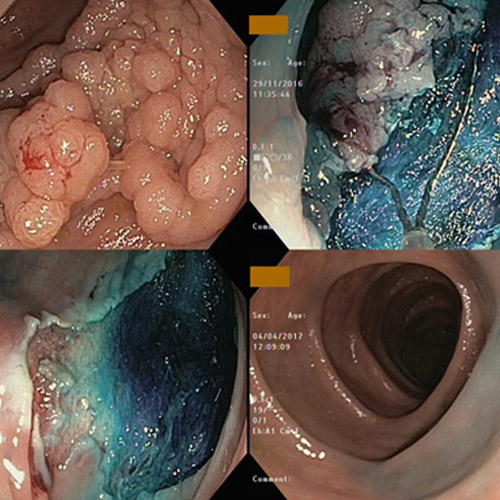
Demonstration of Endoscopic Mucosal Resection Procedure
Top Left: large laterally spreading tumour in the descending colon.
Top Right: following injection of submucosal methylene blue the lesion is sequentially resected using a snare.
Bottom Left: complete resection of the lesion. Procedure duration 45 minutes. Patient went home the same day. Histopathology was a tubulovillous adenoma with focal high grade dysplasia.
Bottom Right: follow up colonoscopy demonstrates no residual adenomatous tissue endoscopically and on biopsies.
Screening
There is extensive high quality evidence that CRC incidence and mortality can be significantly reduced through screening. This is the rationale for the National Bowel Cancer Screening Program, which currently recommends second yearly faecal immunochemical testing (FIT) from 50 to 74 years old for patients at average risk of CRC development (about 95% of the population). The acceptance of FIT by patients is still suboptimal. Primary care physicians can assist in enhancing uptake of FIT by patients. FIT has numerous advantages including low cost and level of invasiveness, repeatability and high sensitivity.
Colonoscopy is the alternative screening modality, either initiated by the health practitioner or in response to a positive FIT. The advantages of colonoscopy include the ability to immediately resect pre-malignant lesions of any size and diagnoses of alternative colorectal pathology. However, it is invasive, associated with a small risk of complications and a relatively expensive screening modality.
Colorectal lesions
The majority of lesions encountered at colonoscopy are pre-malignant, relatively small in size and easily resected. The most common lesions are hyperplastic lesions, adenomas and sessile serrate lesions. Hyperplastic lesions in the distal colorectum are completely benign and do not require surveillance. With improved endoscopic diagnosis a “resect and discard” strategy is likely to be more commonplace for hyperplastic lesions.
Adenomas
Adenomas make up the majority of pre-cancerous lesions as per the conventional adenoma to carcinoma pathway. The prolonged time frame to cancer development allows for ample opportunity to detect and resect pre-cancerous lesions. Adenomas are classified into tubular and tubovillous subtypes, with the villous component conferring a greater risk of progression to CRC.
Sessile serrated lesions
These lesions are being increasingly diagnosed and are histologically distinct from adenomatous lesions They are often in the proximal colon, flat and easily missed. A mucous cap is often the only clue to their detection. The serrated pathway accounts for about 30% of colorectal cancer development. Sessile serrated lesions with a dysplastic component appear to accelerate to CRC faster than conventional adenomas or non-dysplastic sessile serrated lesions.
Advanced lesions
A patient would be considered to have advanced features in the following setting
- three or more adenomas at one colonoscopy
- adenomas greater than 10mm in size
- villous component or high grade dysplasia on histology
Endoscopic assessment
Modern high optical resolution endoscopes now allow for detailed endoscopic assessment and accurate histological prediction in trained hands. Lesions can be viewed with greater magnification and optical filters highlight surface and mucosal structures that guide classification of lesions and the likelihood of submucosal invasion.
Endoscopic resection
The majority of lesions are under 10 mm and only slightly raised. These can be effectively and safely excised using a conventional snare. Conventional snare based polypectomy is more and more moving away from utilising electrocautery, which is associated with delayed bleeding and deeper mural injury.
Lesions beyond 10 mm and especially greater than 20 mm require more enhanced resection techniques. Pedunculated lesions are often pre-treated with a prophylactic modality such as applying clips or injecting adrenaline to the stalk of the polyp. Large flat lesions are termed laterally spreading lesions and require endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD).
EMR is a technique involving injection of a dyed solution to provide a cushion between the mucosal lesion and muscularis and for clarification of tissue layers. A sequential “lift and snare resect” technique is subsequently performed. Lesions up to 20 mm can be excised en bloc whilst multiple resections are required for larger lesions. The risk of post polypectomy bleeding is up to 9% in the proximal and about 3% in the distal colon. Recurrence rates of up to 20 % are often diminutive and easily treated.
ESD is a technique involving a simultaneous injection and subsequent dissection to resect lesions of any size in one piece (en-bloc). Recurrence rates are very low (about 1-5%) but the frequency of immediate complications such as perforation is higher than EMR. The main advantage of ESD is the possibility of cure for superficial colorectal carcinomas.

SkyCity, Suite 212, 20A Lexington Drive, Bella Vista 2153
Phone: 02 8814 1133
Mobile: 0401 978 326
Fax: 02 8814 1988
Send me an Email:
reception@thehillsgastro.com.au
Visit my Website:
thehillsgastro.com.au
Dr Farzan Bahin
MBBS (Hons), FRACP, PhD, MPhil (Med)
Gastroenterologist and Advanced Therapeutic Endoscopist
Consulting from his rooms in Bella Vista and Westmead, Dr Bahin provides high quality ethical and comprehensive patient care covering the breadth of gastroenterology, complex endoscopy and hepatology referrals. He also conducts expedited reviews for urgent cases and fast tracked endoscopic procedures. Dr Bahin treats patients at Blacktown & Mount Druitt Hospitals, Westmead Hospital, Lakeview Private Hospital and Norwest Private Hospital. Routine privately performed procedures do not incur a gap payment.
Dr Bahin has undergone extensive training in large academic hospitals and is accredited for gastroscopy, colonoscopy, ERCP and capsule endoscopy. He is a fellow of the Royal Australasian College of Physicians, a member of the Gastroenterology Society of Australia and the American Society of Gastrointestinal Endoscopy.
Dr Bahin’s strong academic background includes extensive publications, peer review of journals and participation in numerous research trials. He has won numerous prestigious academic awards. He has been awarded his PhD evaluating improvements in complex endoscopy in 2017 and is actively involved as a clinical lecturer for the University of Sydney and Western Sydney University. Special areas of interest include colorectal cancer screening and prevention, therapeutic endoscopy including advanced tissue resection, ERCP, luminal stenting and dilatation.





