When is it time to Consider Obesity (Bariatric) Surgery for your Patient?
Dr Brendan Ryan
MBBS (Hons) FRACS
02 9687 7019
Westmead Specialist Centre,
Suite 9, 16-18 Mons Road,
Westmead 2145
Dr Carolyn Jameson
MBBS BSc(Hons) PhD FRACS
02 9687 7019
Westmead Specialist Centre,
Suite 9, 16-18 Mons Road,
Westmead 2145
If your patient has been unsuccessful losing weight through medical and conservative means, is suffering from the ill-effects of obesity, and meets the criteria on BMI grounds, then an informed discussion about the pros and cons of surgery should be considered.
Eligibility for bariatric surgery (Australian Obesity Management Algorithm):
- Patients with a BMI > 40 kg/m2
- Patients with a BMI > 35 kg/m2 with associated co-morbidities such as diabetes, insulin resistance, hypertension, sleep apnoea, joint disease, fatty liver, PCOS, depression etc.
- Patients with a BMI > 30 kg/m2 with poorly controlled type 2 diabetes and increased cardiovascular risk.
What is the most suitable operation?
There are three operations commonly performed for weight loss in Australia:
- Laparoscopic Sleeve Gastrectomy
- Laparoscopic Gastric Bypass, of which there are two variations:
- a. Roux-en-Y Gastric Bypass
- b. Single Anastomosis Gastric Bypass
- Laparoscopic Gastric Banding. (NB Gastric banding rates have fallen dramatically in Australia and internationally due to poor outcomes in comparison with the Sleeve and Bypass).
Endoscopic procedures for weight loss, such as intra-gastric balloon have poor outcomes long-term as the balloon needs to be removed after six months and has complications. Endoscopic plication is a new variant on an old operation which is only recently TGA approved in Australia with limited efficacy data and no long term data.
Sleeve Gastrectomy
The most common bariatric operation performed is Laparoscopic Sleeve Gastrectomy (LSG). It accounts for 70 per cent of bariatric procedures in Australia. Outcomes in terms of weight loss are excellent with average excess weight loss (EWL) between 60 to 70 per cent and durable over the long term. Furthermore the quality of eating is very good with no vomiting and no alteration in bowel function. The main surgical risk is staple-line leak, which leads to internal infection and re-operation. This risk is less than one per cent.
Even though the sleeve gastrectomy is permanent, there are few long-term issues for patients. There is no increased risk of malignancy or malnutrition. B12 and iron absorption may be lowered and need to be monitored long term. GORD/reflux may be seen in 10 per cent and may require PPI’s.
Gastric Bypass
For severe obesity (BMI > 50) and for patients with diabetes and/or severe co-morbid conditions, gastric bypass must be considered. It has the greatest weight-loss of the common bariatric procedures performed.
There are two common forms of gastric bypass performed in Australia – the Roux-en-Y and the single anastomosis gastric bypass (commonly known as the mini gastric bypass and the Omega Loop gastric bypass). Weight loss is very effective with over 70 per cent EWL.
How does surgery work?
Restriction:
The stomach is made into a small segment approximately 50-100cc in volume. It is completely separated from the rest of the stomach via stapling. The reduced stomach capacity allows patients to become full with small meal portions and therefore allows patients to reduce their caloric intake whilst not feeling hungry. With the gastric sleeve the un-used portion of the stomach is removed from the body at the time of the surgery. With the bypass, the stomach is left inside, retaining its own blood supply but not removed.
Reduced absorption:
In the single anastomoses gastric bypass, a loop of small bowel/intestine is brought up from below and joined to the gastric pouch. This bowel represents the ‘’bypassed’’ length of intestine and varies according to need. It is commonly 150-200cm. This results in the small amount of food eaten not being absorbed to the same degree which assists with weight loss.
If patients have pre-existing severe reflux they are best suited to the Roux-en-Y gastric bypass. This involves a second anastomosis of the small intestine to divert the bile and pancreatic secretions away from the gastric pouch and downstream into a distal segment of small intestine.
What are the risks of gastric bypass?
The gastric bypass has the same initial surgical risks including staple-line leak and bleeding. Once again these have a low incidence of less than one per cent. However, due to the nature of bowel involvement there are some additional considerations with the bypass.
Diarrhoea / Loose stools:
Patients may have loose bowel motions with increased frequency. This is often worse with high fat meals. Patients may complain of two-three loose bowel motions per day. In time, this settles somewhat.
Malnutrition/vitamin deficiency:
Once again B12 and iron absorption are reduced as well as vitamin D. Patients with known osteoporosis are not suitable.
Low protein states can occur.
Dumping:
If sugary foods are consumed, lightheadedness and dizziness may occur. Patients feel hot or flushed and have a need to lie down to obtain relief. Avoiding refined carbohydrates is important.
Small bowel obstruction:
This is seem primarily in the Roux-en-Y bypass and is one of the main advantages for choosing the single anastomises Gastric Bypass over the Roux-en-Y bypass.
Stomach Ulcer:
Smokers are not suitable for gastric bypass.
What can we advise patients with a gastric band?
If you have a patient that has had a gastric band, follow-up with an experienced bariatric clinic is essential. Issues such as insufficient weight loss, vomiting, poor quality of eating and reflux can occur years later.
If the patient is not satisfied with their weight loss or continues to have weight related conditions, a bariatric clinic may be able to investigate and adjust the band. Alternatively, there is now the possibility of removing the gastric band and converting to either the gastric sleeve or bypass. This will result in better quality eating and further weight loss. Patients who are looking for further significant weight loss are advised to convert to the gastric bypass. For patients who long for the ability to eat healthily again, converting to the sleeve is a good option.
Conversion surgery is usually performed as a single stage through our clinic.
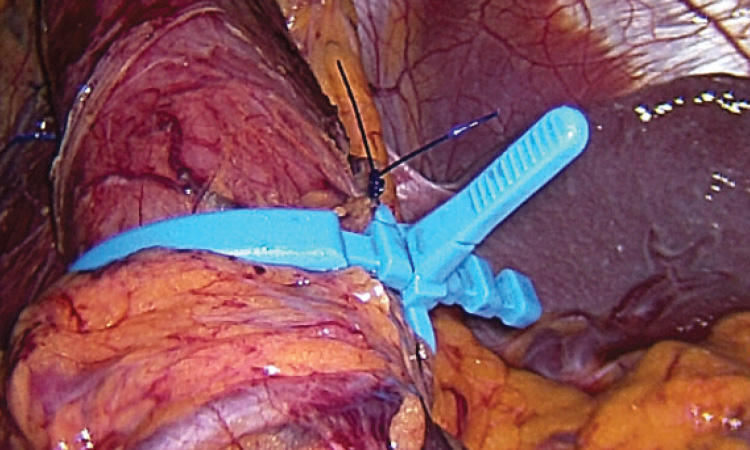
What is the minimizer ring?
This is a new silicon device that can be placed around the gastric pouch of a bypass or sleeve to prevent stretching, one of the causes of late weight regain.
The evidence for the device has been shown in many large studies of patients who have undergone Roux-en-Y gastric bypass and lost more weight than a comparison group of patients who had gastric bypass without the ring.
The main risks of the ring include slip and erosion which have an incidence of less than one per cent. The device is well tolerated by patients and does not usually result in any adverse effects with respect to dysphagia or reflux.
Top five interesting facts about weight loss
- 1. Set-Point theory
One of the reasons patients struggle to keep weight off after diets and exercise is due to the set-point theory where the body vigorously defends its weight. Following acute weight loss, the gut releases chemicals and hormones that drive hunger and increase appetite until the body gets back to its set-point, often re-setting at a higher level. This is why acute dieting not only fails but leaves that individual worse off with increased weight. By contrast both the sleeve gastrectomy and the gastric bypass are operations which physiologically reduce the set point. - 2. Ghrelin, GLP 1 and PYY
Ghrelin is the ‘’hunger hormone’’ that is increased with diet and acute drops in body weight. It stimulates the brain to drive appetite. Studies have shown that Ghrelin levels fall after sleeve gastrectomy and gastric bypass (but not in gastric banding), decreasing the drive to eat. There are many other hormones such as GLP 1 and PYY which are stimulated by the gastric bypass. - 3. Gastric Bypass and long term remission of diabetes
The immediate improvement in diabetic control within days of surgery has been shown not only to be due to the reduced caloric intake but mainly to the enduring physiological changes the surgery produces, which have a long term beneficial effect on diabetes. This is why bariatic surgery is often referred to as metabolic surgery. - 4. High BMI shortens life
Patients with a BMI >40 have a reduction in their life expectancy of 5-7 years, independent of any other co-morbidities. For the first time in history, life expectancy of the community will fall due to the rising incidence of obesity. Bariatric surgery has been shown to improve long term survival. - 5. Severity of obesity is important
The Edmonton Obesity Staging System classifies obesity according to how much it impacts the physical, psychological and functional status of the patient. Some patients with lower BMIs (30-35) may have more metabolically active fat (Metabolic syndrome) and need more aggressive surgical management of their obesity.







